Mirena can be a set‑it‑and‑forget‑it birth control option—but if you’re asking, “What are the long-term side effects of Mirena?" you deserve straight answers.
Over months and years, some users notice persistent spotting, cramping, acne, headaches, breast tenderness, mood or libido changes, and concerns about weight or “hormone imbalance.”
When symptoms linger, it’s easy to wonder: Is this a normal adjustment, a treatable side effect, or a sign the IUD isn’t right for me?
In this doctor‑reviewed guide, we break down evidence, timelines, red flags, and practical next steps—including when to consider removal and what to expect after insertion, replacement, and follow-up.
Hormone type and “mostly local” action
Mirena’s hormone mainly affects the uterine lining (endometrium), making it thinner. Some hormones do reach your bloodstream, which is why some people still get “whole-body” effects like acne or mood changes.
How long does it last?
Depending on current guidance where you live and why you’re using it:
- For pregnancy prevention, Mirena can last up to 8 years in many regions.
- For heavy menstrual bleeding, it’s commonly used for up to 5 years.
What Counts as a Long-Term Side Effect
A “long-term side effect” usually means symptoms that either
- continue after the adjustment phase, or
- show up later (like cysts or device issues), or
- become noticeable over time (like persistent mood changes).
A quick timeline: 0–3 months, 3–12 months, 1+ years
- 0–3 months: spotting, cramps, and irregular bleeding are common.
- 3–12 months: bleeding often gets much lighter; symptoms may settle.
- 1+ years: things are usually stable—unless side effects persist or a device complication develops.
Most Common Long-Term Side Effects
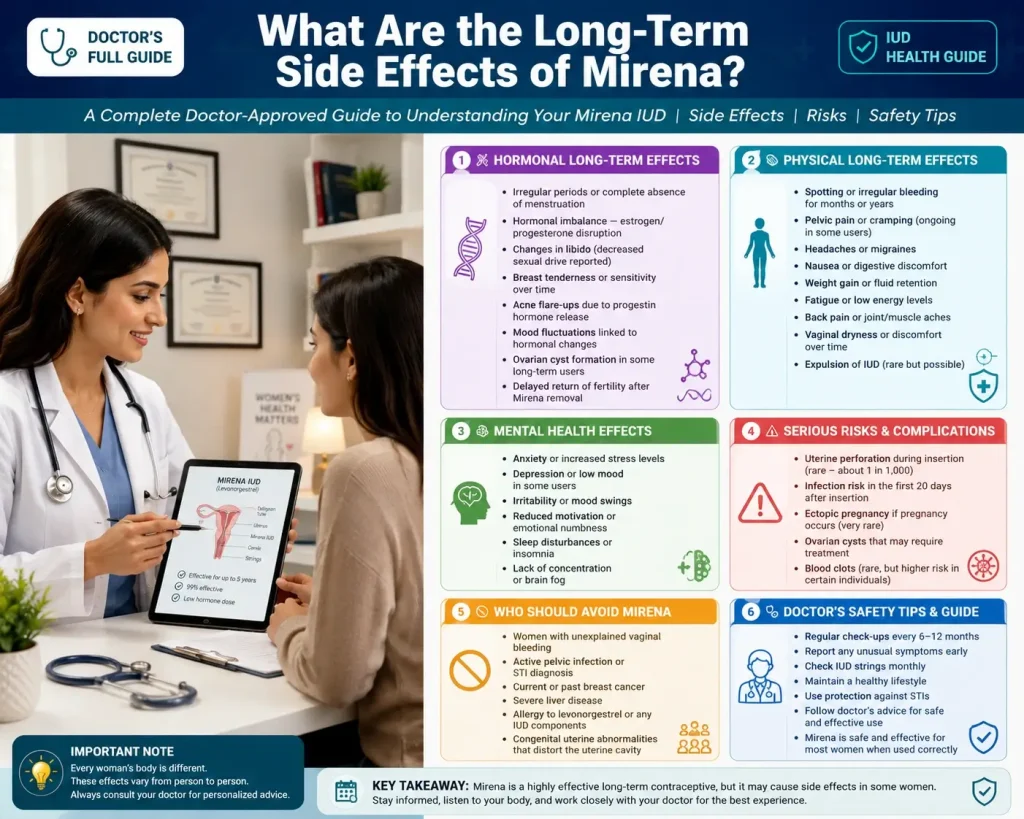
Bleeding changes
This is the biggest long-term “theme” with Mirena.
Lighter periods
Many people have much lighter periods in the long term. This is expected and often the goal—especially if you had heavy bleeding.
Spotting
Some users get on-and-off spotting, even after the first year. It’s often harmless, but if spotting suddenly starts after being stable for a long time, it’s worth checking for the following:
- pregnancy (rare, but possible)
- infection
- An IUD that shifted
- cervical/uterine causes unrelated to Mirena
No period (amenorrhea)
No period on Mirena is usually not dangerous—it’s typically just a very thin uterine lining. Still, if you have pregnancy symptoms, take a test for reassurance.
Mirena can significantly change menstrual cycles, including lighter or absent periods. Some people also explore other reasons behind menstrual cycle changes and delayed periods.
Cramps and pelvic discomfort
Some people have intermittent cramping long-term. Possible reasons include the following:
- The uterus is reacting to the device.
- ovarian cysts
- The IUD is sitting lower than ideal.
- other pelvic issues (fibroids, endometriosis)
If pain is new, sharp, worsening, or linked to sex, get checked.
Hormonal IUDs can sometimes affect vaginal discharge patterns alongside cramping or spotting. Understanding normal vaginal discharge changes during the menstrual cycle may help distinguish harmless symptoms from warning signs.
Some users experience cramping or spotting without regular periods. If this sounds familiar, you may also want to learn more about cramping but no period causes and when they need medical attention.
Hormone-like symptoms
Even though Mirena is mostly local, some people are simply more sensitive to progestins.
Acne
Acne (often jawline/chin) can worsen for some and improve for others. Annoying, yes. Predictable? Not always.
Headaches
Headaches can happen. If you get migraines, track whether they changed after Mirena. Any sudden severe headache or neurological symptoms need urgent evaluation.
Breast tenderness
Breast soreness can come and go, sometimes in cycles—even if you’re not bleeding monthly.
Mood/libido changes
Mood changes (irritability, low mood, anxiety) and lower libido are reported by some users. The tricky part? Sleep, stress, relationships, and life circumstances can look exactly like “hormone symptoms,” so tracking helps.
Hair shedding
Some people notice hair shedding. Because hair loss has many causes (stress, thyroid, and iron deficiency), it’s smart to rule out common culprits instead of assuming Mirena is the only explanation.
Even though Mirena is mostly local, some people are simply more sensitive to progestins. Understanding broader hormonal balance in women can also help explain why side effects vary from person to person.
Weight Gain: Myth vs. Reality
A lot of people blame Mirena for weight gain—and sometimes it truly feels connected.
Here’s the practical truth: research doesn’t consistently show large weight gain caused by Mirena, but individuals can experience the following:
- bloating/fluid retention
- appetite changes
- less activity during months of cramps/spotting
- “life weight gain” that happens over the years anyway
If weight changes are significant and clearly tied to Mirena timing, it’s reasonable to discuss alternatives.
Ovarian Cysts
Ovarian cysts are among the more common Mirena-related findings over time.
Why they happen.
Mirena often doesn’t fully stop ovulation. Sometimes a follicle continues to grow and forms a functional cyst. These are usually benign and temporary.
When they matter
Many cysts cause no symptoms. Get evaluated if you have:
- one-sided pelvic pain
- pain with sex
- persistent bloating/pressure
- sudden severe pain (urgent—could be torsion/rupture)
Infections Over Time
Mirena typically doesn’t cause chronic infection on its own.
Highest-risk window
The highest infection risk related to an IUD is usually around insertion (especially if an STI is present). After that, new infections are more related to exposure risk than the device.
Call a clinician for fever, worsening pelvic pain, foul discharge, or pain during sex.
Device-Related Problems
These are less common, but important because they can cause pain and reduce effectiveness.
Expulsion
The IUD can partially or fully come out. Clues:
- strings suddenly feel longer
- You feel plastic at the cervix.
- cramps/bleeding ramp up again
Embedment
Sometimes the IUD can embed into the uterine wall, leading to persistent pain, bleeding, or difficult removal.
Perforation (rare)
Very rare, usually associated with insertion. It may be found later if the strings aren’t seen or pain persists.
String changes
Strings aren’t a perfect test, but changes matter. If you can’t feel strings (and you used to) or they suddenly feel much longer—especially with pain/bleeding—schedule a check.
Fertility After Mirena
Mirena does not usually cause long-term fertility problems. Most people return to fertility quickly after removal, and you can ovulate before your first period.
If cycles don’t return after a few months, or pregnancy isn’t happening after a reasonable trying period, it’s time to evaluate other factors (thyroid, PCOS, endometriosis, sperm factors, and age).
Safety Questions
Blood clots, blood pressure, and bone health
Because Mirena is progestin-only (and mostly local), it generally doesn’t carry the same clot risk profile as estrogen-containing birth control. It also isn’t known to have major negative effects on bone density, unlike the Depo shot, which can have some negative effects in some users. Blood pressure issues are less typical than with estrogen methods.
Breast cancer (who should avoid hormonal IUDs).
Evidence suggests any risk increase (if present) is generally small in absolute terms for many people, but the decision should be individualized.
People with current breast cancer are usually advised to avoid hormonal contraception, including Mirena. If you have a strong family history or past breast cancer, discuss options with your clinician.
When to Call a Doctor
Red flags
Get urgent medical advice if you have:
- severe or worsening pelvic pain
- fever/chills, foul discharge
- heavy bleeding after a stable pattern
- a positive pregnancy test (important with an IUD)
- missing strings plus pain/bleeding, or you feel the hard plastic
How to Minimise Side Effects
- Give it 3–6 months if symptoms are mild and improving (spotting is common early).
- Track symptoms (mood, headaches, acne, bleeding) for a few weeks—patterns help decisions.
- If pain or bleeding changes suddenly after months/years of stability, ask about an exam and ultrasound to confirm placement.
- If side effects are consistently hurting your quality of life, it’s completely reasonable to discuss removal or switching methods.
Conclusion
The long-term side effects of Mirena are most often about bleeding changes (lighter periods, spotting, or no period) and sometimes hormone-like symptoms (acne, headaches, mood changes, libido shifts, or hair shedding). Less commonly, long-term issues involve ovarian cysts or device-related problems like expulsion or embedment. If something feels “off” after being stable—or if side effects are making daily life harder—getting checked is the fastest way to tell the difference between normal Mirena quirks and problems that need treatment or a change in plan.
FAQs
Can Mirena cause long-term pelvic pain?
It can in some people, especially with cysts, embedment, or if the IUD shifts. New or worsening pain deserves an evaluation rather than waiting it out.
How do I know if my Mirena moved?
Signs include stronger cramps, heavier bleeding, strings that are suddenly longer/shorter, feeling the plastic, or new pain with sex. An exam and ultrasound can confirm placement.
What should I expect after Mirena removal?
Many people have a temporary rebound: more bleeding as cycles restart, acne changes, mood shifts, or headaches for a few weeks. If symptoms are severe or persist for several months, it’s worth evaluating other causes as well.
How common is it to lose your period long-term on Mirena?
Pretty common. Many users have very light bleeding or no period after the first year. It’s usually due to a thin uterine lining, not a dangerous “build-up.”
Do Mirena side effects get worse the longer you have it?
Not usually. Many people find that side effects improve after the first few months. If symptoms worsen later, think about placement changes, cysts, infection, or an unrelated condition—and get checked.