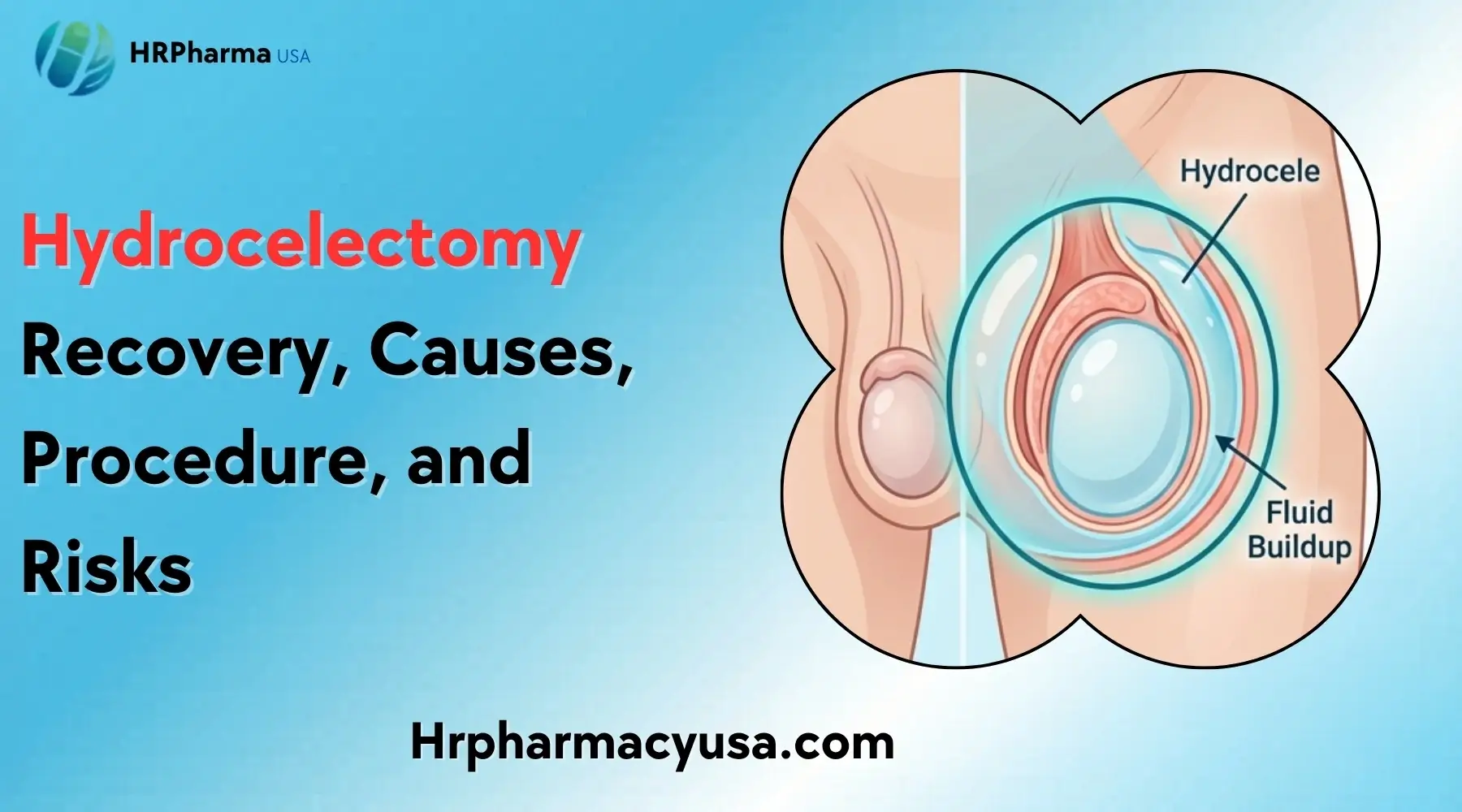
A hydrocele is a fluid-filled sac around a testicle, not the testicle itself, swelling, but fluid collecting in the surrounding area, which can make the scrotum appear enlarged. Usually, it’s painless, but it may feel heavy or uncomfortable, especially when it's large.
The scrotum can swell like a "water balloon" because it fills with fluid.
Picture the testicle as an object inside a thin-lined pouch. If that pouch starts collecting fluid, it’s like slipping the object into a small water balloon. The balloon can expand, feel squishy, and make everything look uneven—without necessarily causing sharp pain.
Hydroceles can be small and barely noticeable or large enough to be annoying when walking, exercising, or even just sitting.
Hydrocele vs. hernia vs. varicocele: quick differences
Scrotal swelling is often caused by a few common conditions that may appear similar at first glance:
- Hydrocele: fluid around the testicle; often smooth, soft, and may feel like it’s filled with water.
- An inguinal hernia occurs when tissue, often part of the intestine, pushes down into the groin or scrotum; this condition can be intermittent and may worsen with activities such as lifting or coughing.
- Varicocele: enlarged veins (like varicose veins) in the scrotum; often described as feeling like a “bag of worms,” more common on the left.
A clinician can usually narrow the diagnosis down quickly, and an ultrasound can confirm it.
Common Causes of Hydrocele
Hydroceles tend to fall into two big categories: in babies/children and in adults. The “why” is often different.
Hydrocele in babies:
In infants, hydroceles are often related to how the groin area develops before birth.
Communicating hydrocele (the open pathway)
A communicating hydrocele means there’s still a small open connection between the abdomen and the scrotum. Fluid can travel down that path and collect around the testicle.
Because fluid shifts, swelling may change throughout the day—smaller in the morning, bigger later, or increasing with crying or straining. This type is more closely related to the risk of inguinal hernia.
Non-communicating hydrocele (fluid trapped in place)
A non-communicating hydrocele means the pathway is closed, but fluid remains trapped around the testicle. Many of these resolve in the first year or two of life, depending on the situation and the clinician’s guidance.
Hydrocele in adults
In adults, hydroceles often develop when scrotal tissues produce excess fluid or when inflammation is triggered, such as by injury or infection.
Inflammation or infection
Inflammation in the scrotum (sometimes from an infection of the epididymis or testicles) can lead to fluid buildup. Treating the underlying problem may help, but occasionally the hydrocele sticks around afterward.
Injury or surgery
Trauma to the groin or scrotum can cause swelling and fluid accumulation. Hydroceles can also appear after certain surgeries in the area, depending on what was done and how tissues heal.
Idiopathic hydrocele (no clear cause)
This condition is very common: everything looks fine, there was no obvious injury, and yet—fluid builds up anyway. “Idiopathic” is just a medical way of saying, “We don’t have a neat explanation.”
Symptoms and When It’s Time to Get Checked
Typical symptoms
Most hydroceles cause symptoms like:
- A painless or mildly uncomfortable scrotal swelling
- A feeling of heaviness or dragging
- Discomfort with walking, exercise, or sex
- Cosmetic concern (yes, that matters too)
The swelling is often smooth and can be one-sided.
Red flags that need urgent evaluation
Some symptoms require prompt evaluation: sudden severe pain, redness, warmth, fever, nausea or vomiting with pain, rapidly enlarging swelling, or a firm lump in or on the testicle.
- Sudden severe pain
- Redness, warmth, fever
- Nausea/vomiting with scrotal pain
- Rapidly enlarging swelling
- A hard lump in or on the testicle
These can point to conditions that need urgent care, like testicular torsion, serious infection, or other causes unrelated to a hydrocele.
How Hydrocele Is Diagnosed
Physical exam and transillumination
A clinician often starts with a physical exam. One classic trick is transillumination—shining a light through the scrotum. Fluid tends to glow, while solid masses don’t.
It’s not a final diagnosis by itself, but it’s a helpful clue.
Scrotal ultrasound
A scrotal ultrasound is the go-to test because it’s quick, painless, and clear. It can:
- Confirm fluid around the testicle.
- Check the testicle itself.
- Look for hernia, masses, varicocele, or other issues.
Ruling out other causes of swelling
The point isn’t just “Yep, there’s fluid.” The point is making sure there isn’t something else going on that needs different treatment.
When Hydrocelectomy Is Recommended
A hydrocelectomy is surgery to remove or repair the sac that’s collecting fluid, aiming for a long-term fix.
When observation is enough
Not every hydrocele needs surgery. Observation may be reasonable when:
- It’s small.
- It’s not painful.
- It isn’t growing.
- There’s no concern for other conditions.
- In infants, spontaneous resolution is expected when the condition is not growing.
When surgery makes sense
At some point, a hydrocele can stop being a “minor nuisance” and start becoming a daily problem.
Pain, heaviness, or lifestyle impact
If it feels like you’re carrying a small water bottle in your underwear all day, that heaviness can wear you down—physically and mentally.
Large or growing hydrocele
A hydrocele that continues to enlarge is unlikely to shrink on its own in adults. Increasing size can mean more discomfort and a more noticeable recovery after surgery—so timing matters.
Concern for underlying issues
Sometimes surgery is recommended because clinicians want a definitive solution after evaluation, especially if there’s any uncertainty or repeated recurrence after other treatments.
Hydrocelectomy Procedure: Step-by-Step
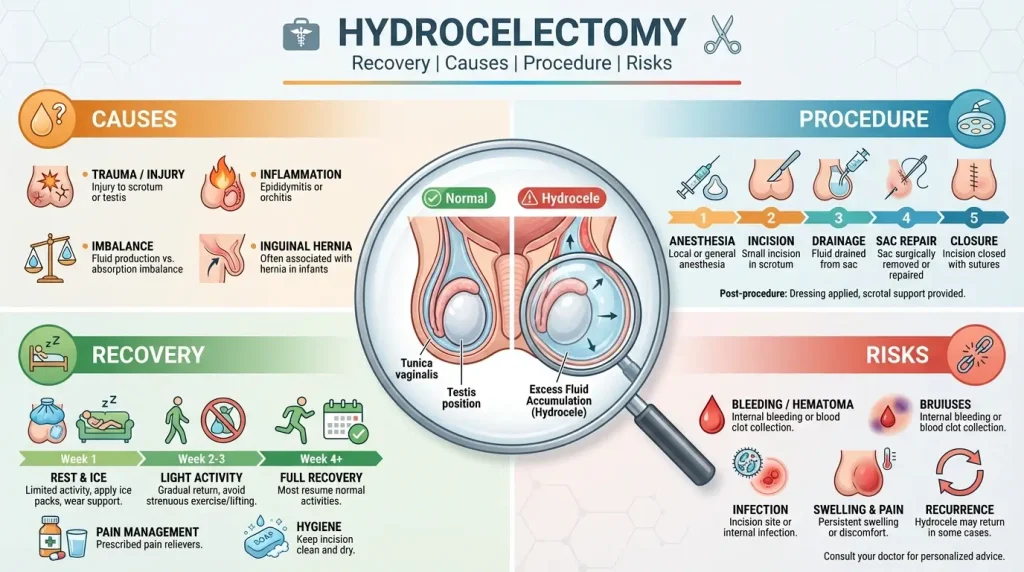
Hydrocelectomy is usually a same-day outpatient surgery, meaning you go home the same day.
Pre-op preparation
Before surgery, you’ll typically have instructions from your surgeon and anesthesia team.
Medications and supplements to discuss
This part matters more than people expect. You’ll be asked about:
- Blood thinners (prescription or over-the-counter)
- NSAIDs
- Supplements that may affect bleeding (some do)
- Other ongoing meds
Please adhere to the provided plan and avoid making assumptions.
Fasting and day-of-surgery checklist
Most people are told not to eat or drink for a specific period before anesthesia. You’ll also want:
- Loose, comfortable clothing
- A ride home
- Supportive underwear is available for after
Anesthesia options
Hydrocelectomy is commonly done under general anesthesia, though some cases may use regional techniques depending on the situation and facility, which can affect the recovery process and the type of supportive underwear recommended for post-operative care.
Surgical approaches
Scrotal approach (common in adults)
In many adult hydrocelectomies, the surgeon makes an incision in the scrotum to access the hydrocele directly.
Inguinal approach (often in children)
In kids—especially when a communicating hydrocele is suspected—the approach may be through the groin to address the pathway that allowed fluid to travel.
What happens during surgery?
Exact details vary, but the overall logic is consistent: stop fluid from re-collecting.
Opening, draining, and reshaping the sac
The surgeon opens the hydrocele sac, drains the fluid, and then modifies the sac so it’s much less likely to refill. There are different surgical techniques for this “reshaping,” and the choice depends on anatomy and the surgeon's preference.
Closing and dressing
The incision is closed, and a dressing is applied. Some cases may involve a drain, but not all. Your surgeon will tell you what to expect.
How long the procedure takes and when to go home
Many hydrocelectomies take roughly 30–90 minutes (varies by complexity). After a recovery-room stay, you’ll go home with instructions about:
- Pain control
- Activity limits
- Showering/bathing
- Follow-up
- Warning signs
Hydrocelectomy Recovery Timeline
Most people have questions about recovery, which takes time even if the surgery is quick.
The first 24–48 hours
These are usually the most “tender” days.
Swelling, bruising, and what’s “normal.”
Expect some swelling and bruising—sometimes a lot more than you’d think for a “small” surgery. The scrotum can look dramatic early on. That doesn’t automatically mean something is wrong.
What matters is the pattern: gradual improvement is beneficial; rapidly worsening pain, spreading redness, fever, or severe swelling needs attention.
Supportive underwear and icing
Support is your best friend here. Supportive underwear helps reduce pulling and movement (which reduces pain). Many surgeons recommend icing in short intervals early on—follow your specific instructions.
In Days 3–7
This period is the “I feel better, but I’m not normal” phase.
Walking, showering, and basic activity
Light walking is often encouraged because it improves circulation and helps prevent stiffness. Showering rules vary—some surgeons allow it after a set time; others want you to wait. Stick to your instructions.
Managing pain and constipation
Pain meds (especially opioids) can cause constipation, and constipation can make you strain, which nobody wants after scrotal surgery. Hydration, fiber, and stool softeners (if recommended) can make this recovery feel 50% easier.
In Weeks 2–4
This phase is when many people start asking, “Can I get back to life now?”
Returning to work
It depends on the job:
- Desk job: often sooner
- Physical job with lifting: often later
You might feel “fine” before your tissues are fully healed. Recovery isn’t just about pain—it’s about preventing setbacks like bleeding or swelling.
Driving, lifting, and exercise
Driving depends on pain control, mobility, and whether you’re taking prescription pain meds. Lifting and exercise are usually restricted for a while because they increase pressure and can worsen swelling or bleeding.
Weeks 4–6 (and beyond)
This phase is where healing starts to feel more complete.
Sex and sports
Many people want a firm date for sex and the gym. The honest answer: it depends on swelling, comfort, incision healing, and your surgeon’s advice. Commonly, restrictions last a few weeks.
Think of it like letting glue cure. It might feel dry on the surface, but it’s still setting underneath.
When results look “final.”
Swelling can linger. Some people look close to normal within a few weeks; for others, it can take longer for the scrotum to fully settle and soften.
Recovery Tips That Actually Help
Wound care and hygiene
Keep the area clean and dry as instructed. Avoid soaking (baths, pools, and hot tubs) until you’re cleared—soaking too early is like inviting bacteria to a party you didn’t plan.
Swelling control
Common, practical tools include:
- Supportive underwear or a jockstrap
- Short icing sessions early (if advised)
- Resting with good positioning
Swelling often behaves unpredictably, but you can guide it towards a more manageable state.
Sleep, positioning, and comfort hacks
Sleeping can be tricky the first few nights. A simple trick: place a pillow under your knees when on your back, or use a small towel roll to prevent uncomfortable shifting. The goal is fewer sudden “ouch” moments.
What to eat and drink for smoother healing
This isn’t glamorous, but it works:
- Plenty of water
- Protein to support tissue repair
- Fiber to prevent constipation
- Go easy on alcohol early on (it can worsen swelling and interact with meds)
Risks and Possible Complications
Hydrocelectomy is generally safe, but it’s still surgery—so risks are real. Knowing them doesn’t make you anxious; it makes you prepared.
Short-term risks
Bleeding and hematoma
A hematoma is a pocket of blood that can collect in the scrotum. It can increase swelling and discomfort and may take time to resolve. Following activity restrictions is a big prevention tool.
Infection
Signs can include increasing redness, warmth, drainage, fever, or worsening pain. Early treatment matters.
Fluid re-accumulation early on
Sometimes swelling after surgery feels like the hydrocele is “back.” Often, it’s just postoperative fluid and inflammation that gradually improve. True recurrence is a different story (more on that below).
Long-term risks
Recurrence
Hydrocelectomy aims to be a long-lasting solution but recurrence can happen. The risk varies based on technique, anatomy, underlying cause, and healing.
Chronic pain or sensitivity
Some people notice prolonged tenderness or sensitivity. Most improve with time, but persistent pain should be evaluated.
Scar tissue
Scar tissue is part of healing, but excessive scarring can occasionally cause discomfort or firmness in the area.
Fertility and testicle safety are common concerns for individuals.
A very common worry is, "Can this mess with fertility or damage the testicle?”
Hydrocelectomy is performed with the goal of protecting the testicle and restoring comfort/normal anatomy. Complications affecting the testicle are uncommon, but any scrotal surgery carries some risk—so choose an experienced urologic surgeon, follow recovery instructions, and attend follow-ups.
Hydrocelectomy vs. Aspiration and Sclerotherapy
Some people ask: “Can’t you just drain it and be done?”
Here’s why aspiration is not typically a permanent solution.
Aspiration removes the fluid with a needle, but it often doesn’t fix the underlying sac that keeps producing or collecting fluid. So the hydrocele can come back—sometimes quickly.
When less invasive options are considered
In certain situations—like people who aren’t viable surgical candidates—clinicians may consider aspiration with sclerotherapy (injecting an agent to reduce recurrence). Results vary, and it may still recur. It’s a “right patient, right scenario” option.
Hydrocelectomy in Children vs. Adults
Key differences in goals and technique
In children, especially with communicating hydroceles, the goal often includes addressing the open pathway that connects the abdomen and scrotum. In adults, the focus is usually on the hydrocele sac itself and preventing re-accumulation.
What parents should expect after surgery?
Kids often bounce back quickly, but they still need the following:
- Pain control (as prescribed)
- Activity limits (yes, even if they feel invincible)
- Wound monitoring
- Follow-up
Swelling can still look impressive for a bit—kids’ bodies heal fast, but they also swell dramatically sometimes.
When to Call Your Surgeon After Hydrocelectomy
Symptoms that shouldn’t be ignored
Call your surgeon or seek urgent evaluation if you notice:
- Fever or chills
- Worsening redness, warmth, or pus-like drainage
- Severe or rapidly increasing pain.
- Scrotum swelling that suddenly escalates
- Trouble urinating
- Shortness of breath, chest pain, or severe dizziness (emergency)
Follow-up visits and what gets checked
Follow-up isn’t just a formality. Your clinician may check:
- Incision healing
- Swelling pattern
- Signs of infection or hematoma
- Whether the hydrocele is resolving as expected
It’s also your chance to ask the practical questions you didn’t think of on surgery day.
Conclusion
Hydrocelectomy is a common, typically outpatient surgery designed to fix a hydrocele for the long haul—especially when swelling becomes uncomfortable, keeps growing, or interferes with everyday life.
The procedure aims to drain the fluid and reshape or remove the sac to prevent it from refilling. Recovery is usually manageable but can be surprisingly “puffy” at first, with swelling and bruising that gradually settle over weeks.
Knowing the causes, understanding the steps of the procedure, and respecting the recovery timeline can make the whole experience feel less like a mystery and more like a plan.
FAQs
Is hydrocelectomy painful?
Expect soreness and tenderness, especially in the first few days. Many people describe it as uncomfortable rather than unbearable. Supportive underwear, rest, and the prescribed pain plan usually make a big difference in managing discomfort after the procedure, helping to alleviate soreness and tenderness during recovery.
Can a hydrocele come back after hydrocelectomy?
Yes, recurrence is possible, though hydrocelectomy is generally considered a durable solution. Following post-op activity restrictions and attending follow-ups helps reduce risk and catch issues early.
How long does hydrocelectomy recovery take?
Most people feel noticeably better within 1–2 weeks, but scrotal swelling can take several weeks to fully settle. Many return to light activities sooner, while heavy lifting and intense exercise often require a longer break based on surgeon guidance.
Do I need a hydrocelectomy right away if I have a hydrocele?
Not always. If it’s small, painless, and not growing, observation may be reasonable. Surgery is more commonly recommended when the hydrocele is large, uncomfortable, growing, or affecting daily life.
When can I exercise or lift weights again after hydrocelectomy?
Light walking is often fine early, but lifting and strenuous workouts usually need to wait several weeks. The exact timing depends on your healing, swelling, and your surgeon’s instructions.